Let’s get one thing straight: calling psyllium husk “nature’s Ozempic” is like calling a bicycle “nature’s Ferrari.” Both move you forward, but the mechanisms, power, and outcomes couldn’t be more different. This comparison isn’t just misleading — it’s scientifically incoherent, and it’s exactly the kind of wellness industry nonsense that keeps patients confused about what actually works.
I’m Dr. James Cole, and I’ve spent three decades explaining metabolism to medical students and patients alike. The psyllium-Ozempic comparison has exploded across social media because it offers people hope for weight loss without needles or prescriptions. But hope built on false premises leads to disappointment and potentially dangerous decisions.
What Ozempic Actually Does to Your Body
Semaglutide (Ozempic, Wegovy) is a GLP-1 receptor agonist that fundamentally rewires your metabolic signaling. It mimics a gut hormone that hits receptors in your pancreas, stomach, brain, and liver simultaneously.
Here’s what happens at the cellular level: GLP-1 agonists bind to specific G-protein coupled receptors that trigger insulin release from pancreatic beta cells while suppressing glucagon from alpha cells. This dual action normalizes blood sugar more effectively than almost any other diabetes medication we have.
But the weight loss mechanism is even more direct. These drugs slow gastric emptying dramatically — food literally sits in your stomach longer. They also cross the blood-brain barrier and activate receptors in the hypothalamus and brainstem that control satiety. Patients on therapeutic doses report that food simply stops being interesting. The neural reward pathway that lights up when you think about pizza? Semaglutide dims that significantly.
According to the STEP 1 trial published in NEJM, patients lost an average of 14.9% of their body weight over 68 weeks on semaglutide 2.4mg versus 2.4% on placebo. That’s not a marginal difference — that’s pharmaceutical-grade metabolic intervention.
What Psyllium Husk Actually Does to Your Body
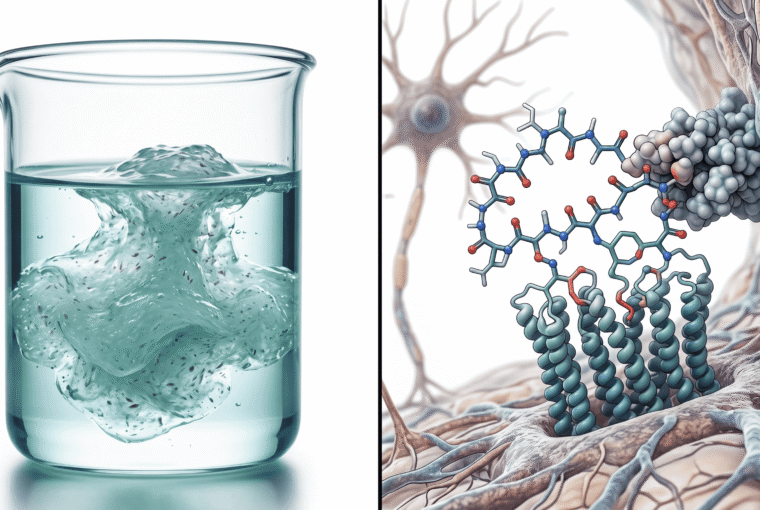
Psyllium is soluble fiber derived from the seeds of Plantago ovata. When it contacts water, it forms a viscous gel — this is not a trivial detail, it’s the entire mechanism.
That gel does three things in your digestive tract. First, it slows carbohydrate absorption in the small intestine, which moderates post-meal blood sugar spikes. Second, it binds to bile acids in your intestines, forcing your liver to pull cholesterol from your bloodstream to make new bile — this is how fiber lowers LDL cholesterol. Third, it adds bulk to stool and feeds beneficial gut bacteria that produce short-chain fatty acids like butyrate.
A 2018 meta-analysis in the American Journal of Clinical Nutrition found that psyllium supplementation (median dose 10.2g daily) reduced fasting blood glucose by 11.1 mg/dL and HbA1c by 0.32% in people with type 2 diabetes. That’s clinically meaningful but nowhere near what GLP-1 agonists achieve.
Regarding weight loss, the data is thin and inconsistent. Most studies show psyllium creates a mild sense of fullness that might reduce caloric intake by 100-150 calories daily if you take it before meals. Over months, this could translate to 2-4 pounds of weight loss maximum. One randomized trial in Appetite (2015) found psyllium supplementation led to 3kg (6.6 lbs) weight loss over 12 weeks versus placebo — but only when combined with caloric restriction.
The Biological Mechanisms Are Completely Different
This is where the comparison falls apart completely. Ozempic works through receptor-mediated hormonal signaling that directly alters brain chemistry and metabolic regulation. It’s pharmacological intervention at the molecular level.
Psyllium works through passive mechanical effects — it’s literally taking up space in your gut and changing the physical properties of your digestive contents. It doesn’t bind to receptors, it doesn’t cross into your bloodstream in meaningful amounts, and it absolutely doesn’t alter neural reward pathways in your brain.
To claim these are comparable is like saying a sponge and a computer both process information because a sponge absorbs water and a computer processes data. The superficial similarity (both involve “processing”) masks fundamental differences in mechanism and capability.
What the Media Consistently Gets Wrong
Wellness journalism loves finding “natural alternatives” to pharmaceuticals because it fits a narrative that nature is always gentler and safer. But this framing is intellectually dishonest on multiple levels.
First, “natural” doesn’t mean “effective” or “safe.” Arsenic is natural. Botulinum toxin is natural. Efficacy and safety are determined by mechanism and dose, not source.
Second, the media consistently conflates correlation with causation. Yes, populations that eat more fiber have lower rates of obesity and metabolic disease. But they also eat less processed food, move more, sleep better, and have different stress profiles. You can’t extract fiber from that complex matrix and expect it to carry all those benefits.
Third — and this is critical — the comparison sets up false expectations. When patients try psyllium expecting Ozempic-like results and don’t get them, they become cynical about legitimate dietary interventions. I’ve seen patients abandon evidence-based nutrition entirely because fiber supplements didn’t deliver on the overinflated promises they’d read online.
The WHO guidelines on obesity management mention fiber as one component of a comprehensive dietary approach, not as a standalone intervention comparable to pharmacotherapy. That context matters.
When Psyllium Actually Helps (And When It Doesn’t)
Here’s what I tell my patients: psyllium is genuinely useful for specific clinical indications, but weight loss isn’t really one of them.
It’s excellent for chronic constipation — the evidence here is robust. Taking 5-10 grams daily increases stool frequency and softness reliably. It also helps with IBS-C (constipation-predominant irritable bowel syndrome) by normalizing bowel transit time.
For cholesterol management, psyllium reduces LDL by approximately 5-10% when taken consistently at 7+ grams daily. This is meaningful but modest compared to statins, which reduce LDL by 30-50%. Still, for patients who can’t tolerate statins or need additional LDL reduction, psyllium is a legitimate evidence-based option.
For blood sugar control in type 2 diabetes, psyllium modestly improves glycemic control as an adjunct to other interventions. The American Diabetes Association standards of care mention fiber supplementation as a reasonable consideration, but it’s listed alongside other dietary modifications, not as a standalone therapy.
Where psyllium doesn’t help: rapid weight loss, appetite suppression comparable to GLP-1 agonists, reversing metabolic syndrome, or treating obesity as a primary intervention. If you’re hoping to lose 15-20% of your body weight through fiber supplements alone, you’re going to be disappointed.
The Real Comparison: Fiber vs. GLP-1 Agonists by the Numbers
Let me give you the clinical data side by side, because numbers don’t lie even when headlines do.
Average weight loss over one year: Semaglutide 2.4mg produces 15-17% body weight reduction. Psyllium 10-15g daily produces 1-3% body weight reduction, and that’s being generous with the data.
HbA1c reduction in type 2 diabetes: Semaglutide reduces HbA1c by 1.5-2%. Psyllium reduces it by 0.3-0.5%.
Cost: Semaglutide costs $900-1,300 monthly without insurance. Psyllium costs $10-20 monthly for therapeutic doses.
Side effects: Semaglutide causes nausea in 40-50% of patients, with 5-7% discontinuing due to GI side effects. Psyllium causes bloating and gas in 10-15% of users, rarely severe enough to discontinue.
The cost-benefit calculation is completely different for these interventions. Psyllium is low-risk, low-cost, and produces modest benefits that compound over time. GLP-1 agonists are high-cost, higher-risk, but produce dramatic results that can be life-changing for people with obesity and metabolic disease.
What You Should Actually Do
If you’re considering psyllium because you saw it called “nature’s Ozempic,” let me reframe this for you.
Use psyllium if you need help with constipation, want to modestly improve your cholesterol profile, or need better glycemic control as part of comprehensive diabetes management. Take 5-10 grams daily mixed in at least 8 ounces of water, and drink another glass of water immediately after. Start with half doses for the first week to let your gut bacteria adjust.
Don’t use psyllium as a weight loss strategy or Ozempic substitute. If you need significant weight loss for health reasons, talk to your doctor about comprehensive medical weight management, which might include GLP-1 agonists, or metabolic surgery depending on your situation.
Here’s what actually works for sustainable weight management according to NIH guidelines: caloric restriction combined with increased physical activity, behavioral therapy to address eating patterns, adequate protein intake (0.7-1g per pound of ideal body weight), resistance training to preserve muscle mass, and sufficient sleep (7-9 hours nightly).
Fiber should be part of that picture — not from supplements primarily, but from whole foods. Vegetables, legumes, whole grains, and fruits deliver fiber alongside thousands of other bioactive compounds that work synergistically. Eating 25-35 grams of fiber daily from whole foods is genuinely beneficial for metabolic health, cardiovascular protection, and probably colorectal cancer prevention.
The Bigger Problem With Miracle Cure Narratives
The “nature’s Ozempic” framing represents something larger and more troubling in health communication: the relentless search for simple solutions to complex biological problems.
Obesity is a chronic disease involving hormonal dysregulation, neural reward pathway dysfunction, genetic predisposition, environmental factors, sleep disruption, stress response abnormalities, and often psychological trauma. Fiber addresses exactly one tiny piece of this puzzle — the mechanical slowing of nutrient absorption.
When we pretend that a single supplement can substitute for comprehensive pharmaceutical intervention, we’re not empowering patients — we’re setting them up for failure and self-blame. I’ve watched patients spend years trying various “natural” approaches to weight loss, getting progressively more frustrated, when they would have benefited from medical treatment years earlier.
The shame and stigma around obesity medications is part of the problem. Patients feel like they’ve “failed” if they need pharmaceutical help, so they keep searching for natural alternatives that will let them avoid that psychological burden. But diabetes medications aren’t moral failures, and neither are obesity medications.
One Final Word on Internet Health Trends
Social media has democratized health information in some valuable ways, but it’s also created an environment where catchy comparisons spread faster than accurate science.
When you see claims like “nature’s [pharmaceutical name],” your skepticism should spike immediately. These comparisons are almost always marketing language designed to sell supplements or generate clicks, not clinical assessments based on comparable efficacy data.
Real medical science is usually less exciting and more nuanced. Fiber is good for you in modest ways that compound over decades. GLP-1 agonists are powerful tools with significant side effects that work dramatically in months. These aren’t competing alternatives — they’re different categories of intervention entirely.
Your one actionable takeaway: Stop looking for natural pharmaceuticals and start building actually sustainable health practices — eat 25+ grams of fiber daily from whole foods, walk 30 minutes most days, sleep 7-9 hours nightly, and if you need medical weight management, pursue it without shame through proper clinical channels.