The Medical Establishment Has Been Lying By Omission
Let me start with something that will make both cannabis advocates and prohibitionists uncomfortable: nearly everything you’ve been told about marijuana is either outdated, oversimplified, or deliberately misleading. As a physician who’s reviewed the actual clinical literature—not SAMHSA press releases or dispensary marketing—I can tell you the truth is far more nuanced than “weed is harmless” or “cannabis destroys brains.”
The FDA classifies cannabis as Schedule I, claiming it has “no accepted medical use.” Yet 38 states have legalized medical marijuana, and the NIH now funds clinical trials studying its therapeutic applications. This isn’t about legalization politics—it’s about understanding what cannabis actually does to human physiology.
How Cannabis Actually Works In Your Body
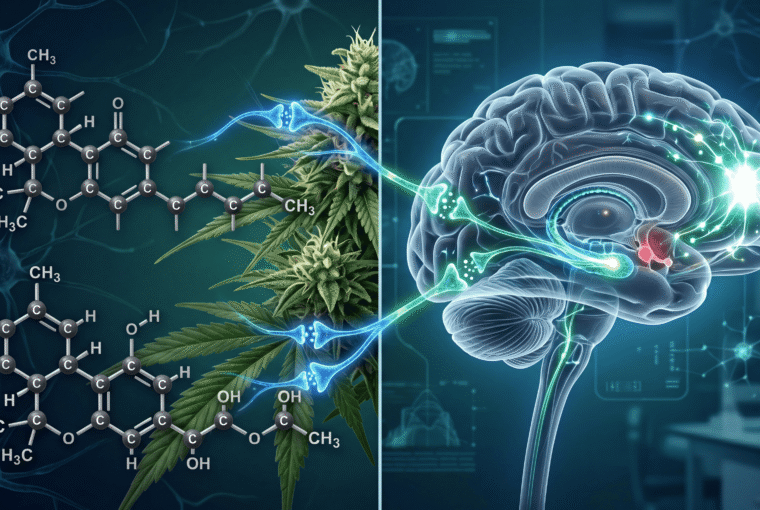
Cannabis contains over 100 cannabinoids, but two matter most clinically: THC (delta-9-tetrahydrocannabinol) and CBD (cannabidiol). Here’s the mechanism the media consistently botches: these compounds interact with your endocannabinoid system—a network of CB1 and CB2 receptors throughout your brain, immune system, and organs.
THC binds directly to CB1 receptors in your brain’s hippocampus, amygdala, and prefrontal cortex. This explains the cognitive effects: CB1 activation in the hippocampus disrupts short-term memory formation. In the amygdala, it modulates fear and anxiety responses. In the prefrontal cortex, it impairs executive function and decision-making.
CBD works differently—it’s a negative allosteric modulator, meaning it changes the shape of CB1 receptors without directly binding to them. This is why CBD doesn’t get you high and may actually counteract some THC effects. The 2021 study in Neuropsychopharmacology showed CBD reduces THC-induced anxiety by preventing excessive CB1 activation.
The Real Health Benefits (With Actual Evidence)
Let’s address what cannabis can legitimately treat, based on clinical trials—not testimonials or dispensary claims. The evidence is strongest for chronic pain, particularly neuropathic pain where opioids fail. A New England Journal of Medicine study demonstrated that vaporized cannabis reduced neuropathic pain intensity by 30% in HIV patients—comparable to gabapentin without the sedation.
For chemotherapy-induced nausea, synthetic THC (dronabinol) has FDA approval because it works through a clear mechanism: activating CB1 receptors in the brainstem’s vomiting center. It’s not a first-line treatment, but for patients who’ve failed ondansetron and other antiemetics, cannabis-based medications provide relief when nothing else does.
Multiple sclerosis spasticity responds to nabiximols (Sativex in Europe), a 1:1 THC:CBD oral spray. The Lancet Neurology trial showed significant reduction in patient-reported spasticity scores. The mechanism? CB1 activation reduces neurotransmitter release at spinal cord synapses, decreasing muscle spasm signals.
For epilepsy—specifically Dravet and Lennox-Gastaut syndromes—CBD (Epidiolex) has robust evidence. It reduces seizure frequency by approximately 40% in treatment-resistant cases. The exact mechanism remains under investigation, but likely involves CBD’s effects on voltage-gated sodium channels and GPR55 receptors, independent of the endocannabinoid system.
The Side Effects Nobody Wants To Discuss
Now for what the cannabis industry downplays and what prohibitionists exaggerate. Acute cognitive impairment is real and dose-dependent. THC temporarily reduces hippocampal activity, impairing memory encoding for 2-4 hours post-use. If you’re studying, working, or driving, this matters—your brain literally cannot form new memories as efficiently.
Cardiovascular effects are underappreciated. THC causes tachycardia and increases myocardial oxygen demand through CB1-mediated sympathetic activation. For healthy young adults, this is trivial. For someone with coronary artery disease, it increases acute coronary syndrome risk. A 2023 American Heart Association study found daily cannabis use increased heart attack risk by 34%.
Cannabis hyperemesis syndrome is bizarre but real—paradoxically, chronic heavy use causes cyclic vomiting that only hot showers temporarily relieve. We don’t fully understand why, but it likely involves CB1 receptor downregulation in the gut and altered thermoregulation. It resolves with abstinence but recurs with resumed use.
Psychiatric risks depend entirely on pre-existing vulnerability. If you have family history of schizophrenia or bipolar disorder, high-potency THC products (>15%) increase psychosis risk. The mechanism: excessive CB1 activation disrupts prefrontal-striatal dopamine regulation. The Lancet Psychiatry 2019 study found daily high-potency use increased psychosis odds fivefold.
The Adolescent Brain Question
This is where I break from both extremes. Yes, adolescent cannabis use affects neurodevelopment—but the magnitude matters. Your prefrontal cortex doesn’t finish myelinating until age 25. Heavy THC exposure during this period alters white matter tract development and may reduce adult IQ by 6-8 points, according to Duke University’s longitudinal study.
But “heavy use” means near-daily use for years, not trying it a few times in college. The brain is resilient—occasional use doesn’t permanently damage neurocognitive function. The risk-benefit calculation for a 16-year-old experimenting versus a 40-year-old cancer patient using medical cannabis is completely different.
What The Media Consistently Gets Wrong
The biggest myth: “cannabis is either completely safe or extremely dangerous.” Both are false. Cannabis is a pharmacologically active substance with therapeutic applications and legitimate risks. Treating it as harmless ignores cardiovascular and psychiatric complications. Treating it as equivalent to heroin ignores its lower addiction potential (9% versus 25%) and absence of lethal overdose risk.
Second myth: “natural means safe.” Arsenic is natural. Botulinum toxin is natural. “Natural” tells you nothing about safety or efficacy. What matters is dose, frequency, delivery method, and individual biology. Vaporized medical cannabis for MS is not the same as smoking blunts of 30% THC flower recreationally.
Third myth: “CBD is the good cannabinoid, THC is the bad one.” This oversimplification misses how they work synergistically. CBD alone doesn’t effectively treat many conditions that respond to full-spectrum cannabis. The entourage effect hypothesis suggests cannabinoids, terpenes, and flavonoids work together—though this needs more rigorous testing.
The Addiction Reality
Cannabis use disorder is real but misunderstood. About 9% of users develop dependence—far lower than alcohol (15%) or nicotine (32%), but not zero. The mechanism involves CB1 receptor downregulation with chronic use, creating tolerance and withdrawal symptoms: irritability, insomnia, decreased appetite, and anxiety.
These symptoms peak 2-6 days after cessation and resolve within 2 weeks—much milder than alcohol or benzodiazepine withdrawal, which can be life-threatening. But psychological dependence can be profound. If you need cannabis to sleep, eat, or feel normal, that’s a problem regardless of whether it causes physical withdrawal.
Pregnancy And Cannabis: The Uncomfortable Truth
This is where I lose the “cannabis is harmless” crowd. THC crosses the placenta and disrupts fetal brain development. It interferes with endocannabinoid signaling that guides neuronal migration and synapse formation. NIH research shows prenatal exposure associates with lower birth weight, preterm delivery, and childhood attention problems.
The “but it helps my nausea” argument doesn’t justify the risk. We have safer antiemetics. Using cannabis during pregnancy is prioritizing maternal comfort over fetal neurodevelopment—a trade-off I can’t medically support.
What You Should Actually Do
If you’re considering cannabis for medical purposes: Start with your actual diagnosis. Cannabis isn’t a cure-all—it has specific therapeutic applications. For chronic pain, try it after NSAIDs and physical therapy, not before. For anxiety, cognitive behavioral therapy has better long-term outcomes than daily THC use, which often worsens anxiety over time.
Choose products with known CBD:THC ratios. Higher CBD content (2:1 or 1:1) provides therapeutic benefits with fewer cognitive effects. Avoid synthetic cannabinoids (K2, Spice)—these are not safer alternatives; they’re significantly more dangerous due to unpredictable receptor binding and potency.
If you use recreationally: Limit frequency to avoid tolerance and dependence. Skip use entirely if you have personal or family history of psychosis or substance use disorders. Never drive within 4 hours of use—THC impairs reaction time regardless of how “fine” you feel. And if you’re under 25, understand you’re using a substance while your brain is still developing. That doesn’t mean don’t do it, but make an informed choice.
For policymakers and parents: Legalization doesn’t equal endorsement. We legalize alcohol despite clear harms because prohibition failed. Regulation beats black markets, where products have unknown potency and contaminants. Education should be honest—exaggerated dangers create credibility gaps that lead youth to dismiss legitimate risks.
The Bottom Line
Cannabis is neither the miracle cure advocates claim nor the brain-destroying poison prohibitionists warn about. It’s a complex pharmacological agent with legitimate medical applications, real side effects, and meaningful risks for vulnerable populations. The conversation needs to move beyond “legal versus illegal” to “appropriate versus inappropriate use.”
As a physician, my job isn’t to tell you whether to use cannabis—it’s to give you the information to make an intelligent decision. The data exists. The mechanisms are understood. What we need now is honest discussion replacing both corporate marketing and outdated propaganda.
Your power lies in understanding that cannabis affects biology in specific, measurable ways—and those effects are neither uniformly beneficial nor universally harmful.